- Record: found
- Abstract: found
- Article: not found
Implementation and Postoperative Management of Continuous Adductor Canal Catheters for Total Knee Arthroplasty to Reduce Surgical Backlog of the COVID-19 Pandemic: An Acute Pain Service Nursing Perspective and Educational Resource
Read this article at
Abstract
Purpose
In response to the surgical backlog created by the COVID-19 pandemic and to spare valuable hospital resources, we developed and implemented a continuous adductor canal catheter (CACC) program for total knee arthroplasty (TKA) patients. CACC's offer superior analgesia, decrease opioid use, increase patient satisfaction while simultaneously promoting a decrease length of hospital stay, and even same day discharges. The implementation of analgesia protocols utilizing continuous peripheral nerve catheters and isometric pumps has been described for other surgical procedures and populations, however the role of the Acute Pain Service Nurse (APS RN) in the implementation of such a program has not been described in the literature.
Design
An initiative for TKA patients receiving CACC was developed and implemented for patients recovering both in the hospital and at home.
Methods
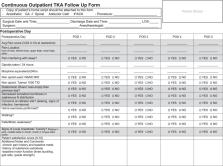
We describe the development and implementation of a CACC program for TKA patients in response to the surgical backlog created by the COVID-19 pandemic from the perspective of the APS RN. We provide a detailed narrative description of our postoperative assessment and experience and offer practical insights for the postoperative care of these patients. We share the educational resources and assessment tools we developed to ensure consistent, safe, and effective clinical management of CACC patients in the hospital and at home.
Findings
CACCs via elastomeric pumps have been shown to offer significant advances to pain control following TKA, decrease opioid use, enable earlier discharge, and improve patient satisfaction, all of which we observed unequivocally in our patients. In our experience, implementation of daily telephone follow up by an APS RN for discharged TKA patients with a CACC was crucial for patient safety, patient satisfaction and reducing emergency phone calls and emergency room visits.
Related collections
Most cited references25
- Record: found
- Abstract: found
- Article: not found
Pain assessment.

- Record: found
- Abstract: found
- Article: found
Local anesthetic systemic toxicity: current perspectives
- Record: found
- Abstract: found
- Article: not found
