- Record: found
- Abstract: found
- Article: found
Medical students’ perspectives of their clinical comfort and curriculum for acute pain management
Abstract
Objectives
Acute pain is a common presenting complaint in health care. Yet, undertreatment of pain remains a prevailing issue that often results in poor short- and long-term patient outcomes. To address this problem, initiatives to improve teaching on pain management need to begin in medical school. In this study, we aimed to describe medical students’ perspectives of their curriculum, comfort levels, and most effective pain teaching modalities.
Materials and methods
A cross-sectional, online survey was distributed to medical students at the University of Alberta (Edmonton, Canada) from late May to early July 2015. Data were collected from pre-clerkship (year 1 and 2) and clerkship (year 3 and 4) medical students for demographic characteristics, knowledge, comfort, and attitudes regarding acute pain management.
Results
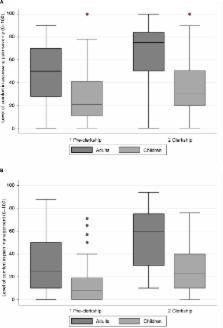
A total of 124/670 (19.6%) surveys were returned. Students recalled a median of 2 (interquartile range [IQR]=4), 5 (IQR=3.75), 4 (IQR=8), and 3 (IQR=3.75) hours of formal pain education from first to forth year, respectively. Clerkship students were more comfortable than pre-clerks with treating adult pain (52.1% of pre-clerks “uncomfortable” versus 22.9% of clerks, p<0.001), and overall, the majority of students were uncomfortable with managing pediatric pain (87.6% [64/73] pre-clerks and 75.0% [36/48] clerks were “uncomfortable”). For delivery of pain-related education, the majority of pre-clerks reported lectures as most effective (51.7%), whereas clerks chose bedside instruction (43.7%) and small group sessions (23.9%). Notably, 54.2%, 39.6%, and 56.2% of clerks reported incorrect doses of acetaminophen, ibuprofen, and morphine, respectively, for adults. For children, 54.2%, 54.2%, and 78.7% of clerks reported incorrect doses for these same medications.
Most cited references22
- Record: found
- Abstract: not found
- Article: not found
A guide for the design and conduct of self-administered surveys of clinicians.
- Record: found
- Abstract: found
- Article: not found
Causes and consequences of inadequate management of acute pain.
- Record: found
- Abstract: found
- Article: not found