- Record: found
- Abstract: found
- Article: found
Metastatic Squamous Cell Carcinoma from Lung Adenocarcinoma after Epidermal Growth Factor Receptor Tyrosine Kinase Inhibitor Therapy
brief-report
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
Inhibition of mutated epidermal growth factor receptor (EGFR), EGFR tyrosine kinase
inhibitor (TKI), is one of the most successful cancer targeted therapies [1]. While
this therapy has been beneficial for many non-small cell lung cancer (NSCLC) patients
with activated EGFR mutations, almost all patients inevitably develop acquired resistance
which limits the median response duration to around 1 year [2]. Most of the mechanisms
leading to EGFR TKI resistance are additional mutation or amplification of alternative
pathways, and morphological transformation to small cell lung cancer (SCLC) [3].
Recently, several authors reported another type of morphologic transformation for
EGFR TKI resistance, namely, transformation from adenocarcinoma to squamous cell carcinoma
[4-6]. However, the reports were of limited value because they were based only on
biopsied specimens. This report describes a case of lung adenocarcinoma with transformation
to squamous cell carcinoma that was established histological evaluation of lobectomy
specimen.
CASE REPORT
A 40-year-old man with a 23-year smoking history received a medical check-up, which
revealed a solitary pulmonary nodule. Chest computed tomography revealed a 17-mm-sized
tumor at the peripheral posterior segment of the right upper lobe (clinically T1aN0M0).
The patient underwent a right upper lobectomy with mediastinal lymph node dissection.
Histological examination showed a 1.3-cm-sized poorly differentiated adenocarcinoma
with solid and acinar growth patterns with visceral pleural invasion and no lymph
node metastasis (pT2aN0). The tumor cells showed marked nuclear atypia, numerous mitoses
(23/10 high power field [HPF]) and multifocal microscopic necrosis. The tumor was
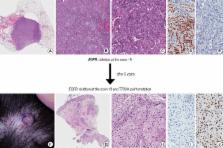
dissected and entirely embedded. We morphologically and immunohistochemically evaluated
all tumor sections to rule out the possibility of adenosqumous carcinoma (Fig. 1A–E).
The patient received adjuvant chemotherapy with combined vinorelbine and cisplatin.
Four years later, multiple metastatic lesions were found at the right lower lobe,
right pleura, right fifth rib, and right femoral head. EGFR mutation analysis, using
a previously resected lobectomy specimen, revealed a deletion at exon 19 of the EGFR
gene. The patient was treated with afatinib, which is an EGFR TKI and radiation therapy.
The patient showed partial remission of the tumor.
Two years later, the patient developed multiple metastatic lesions throughout the
body, including a telangiectatic nodule on the scalp. A punch biopsy was performed
and histologic evaluation of the biopsied specimen showed a tumorous lesion in the
deep dermis. This tumor showed squamoid appearance with sheet-like growth patterns
and evident intercellular bridges. Compared to the previous lobectomy specimen, the
tumor cells were more bland with moderate nuclear atypia, some mitotic activity (13/10
HPF) and no necrosis. Immunohistochemical staining showed diffuse and strong p63 immunoreactivity
and no thyroid transcription factor 1 immunoreactivity (Fig. 1F–J). EGFR mutation
analysis, using a biopsied specimen, revealed a deletion at exon 19 of the EGFR gene
and an additional T790M point mutation. After several special and immunohistochemical
stainings, this tumor was diagnosed as a metastatic carcinoma from the lung with squamous
differentiation. The patient informed consent was waived by the Institutional Review
Board of the Samsung Medical Center (2016-08-109).
DISCUSSION
Lung cancer is the most common cause of cancer deaths in Korea [7]. Traditional therapy,
including resection, platinum-based chemotherapy and radiation therapy, have only
limited therapeutic value. Therefore, the 5-year survival rate of lung cancer has
not changed significantly in the past 30 years [8].
EGFR TKI therapy, which specifically targets EGFR, was recently introduced and provided
guidance in this situation. Targeting EGFR in patients with activating EGFR mutations
has shown initial and significant success in practice [1]. Unfortunately, the vast
majority of patients develop resistance to the treatment, typically in less than 1
year. In this situation, understanding the mechanism of the resistance became very
important.
Most of the mechanisms that lead to EGFR TKI resistance involve an additional mutation,
such as a T790M mutation, or amplification of alternative pathways. In addition, morphological
transformation is also a well-known mechanism. The most well known example of this
interesting phenomenon is the transformation from NSCLC to SCLC [9].
Recently, several authors have described histologic transformation from lung adenocarcinoma
to squamous cell carcinoma as a mechanism of resistance to EGFR TKI therapy [4-6].
In four previously reported cases, all four patients were female and three of them
had never been smokers. The most common EGFR mutation was an L858R point mutation
and the most common acquired gene alteration was a T790M point mutation. All cases
showed the same EGFR mutation in both primary and metastatic carcinomas.
The mechanism of this morphologic transformation is still poorly understood. Possible
explanations include (1) small population of squamous cell carcinoma phenotype cells
are already present before the EGFR TKI therapy and selectively survive during EGFR
TKI therapy; or (2) carcinoma cells acquire a different morphologic phenotype during
EGFR TKI therapy [6].
Considering that primary adenosquamous carcinoma shows the same mutations in both
adenocarcinoma and squamous cell carcinoma components, additional studies are needed
and a solution is beyond the scope of this report.
In conclusion, lung primary adenocarcinoma can transform into squamous cell carcinoma
after EGFR TKI therapy. We should be aware of this phenomenon to avoid misdiagnosis
in practice.
Related collections
Most cited references8
- Record: found
- Abstract: found
- Article: not found
Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2012.
Kyu-Won Jung, Young-Joo Won, Hyun-Joo Kong … (2015)
- Record: found
- Abstract: found
- Article: not found
Known and putative mechanisms of resistance to EGFR targeted therapies in NSCLC patients with EGFR mutations-a review.
Erin L Stewart, Samuel Tan, Geoffrey Liu … (2015)

- Record: found
- Abstract: found
- Article: found
Transformation to Small Cell Lung Cancer of Pulmonary Adenocarcinoma: Clinicopathologic Analysis of Six Cases
Soomin Ahn, Soo Hyun Hwang, Joungho Han … (2016)