- Record: found
- Abstract: found
- Article: found
Homelessness, unstable housing, and risk of HIV and hepatitis C virus acquisition among people who inject drugs: a systematic review and meta-analysis
Read this article at
Summary
Background
People who inject drugs (PWID) are at increased risk for HIV and hepatitis C virus (HCV) infection and also have high levels of homelessness and unstable housing. We assessed whether homelessness or unstable housing is associated with an increased risk of HIV or HCV acquisition among PWID compared with PWID who are not homeless or are stably housed.
Methods
In this systematic review and meta-analysis, we updated an existing database of HIV and HCV incidence studies published between Jan 1, 2000, and June 13, 2017. Using the same strategy as for this existing database, we searched MEDLINE, Embase, and PsycINFO for studies, including conference abstracts, published between June 13, 2017, and Sept 14, 2020, that estimated HIV or HCV incidence, or both, among community-recruited PWID. We only included studies reporting original results without restrictions to study design or language. We contacted authors of studies that reported HIV or HCV incidence, or both, but did not report on an association with homelessness or unstable housing, to request crude data and, where possible, adjusted effect estimates. We extracted effect estimates and pooled data using random-effects meta-analyses to quantify the associations between recent (current or within the past year) homelessness or unstable housing compared with not recent homelessness or unstable housing, and risk of HIV or HCV acquisition. We assessed risk of bias using the Newcastle-Ottawa Scale and between-study heterogeneity using the I 2 statistic and p value for heterogeneity.
Findings
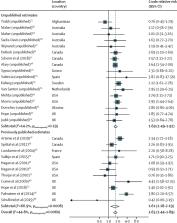
We identified 14 351 references in our database search, of which 392 were subjected to full-text review alongside 277 studies from our existing database. Of these studies, 55 studies met inclusion criteria. We contacted the authors of 227 studies that reported HIV or HCV incidence in PWID but did not report association with the exposure of interest and obtained 48 unpublished estimates from 21 studies. After removal of duplicate data, we included 37 studies with 70 estimates (26 for HIV; 44 for HCV). Studies originated from 16 countries including in North America, Europe, Australia, east Africa, and Asia. Pooling unadjusted estimates, recent homelessness or unstable housing was associated with an increased risk of acquiring HIV (crude relative risk [cRR] 1·55 [95% CI 1·23–1·95; p=0·0002]; I 2= 62·7%; n=17) and HCV (1·65 [1·44–1·90; p<0·0001]; I 2= 44·8%; n=28]) among PWID compared with those who were not homeless or were stably housed. Associations for both HIV and HCV persisted when pooling adjusted estimates (adjusted relative risk for HIV: 1·39 [95% CI 1·06–1·84; p=0·019]; I 2= 65·5%; n=9; and for HCV: 1·64 [1·43–1·89; p<0·0001]; I 2= 9·6%; n=14). For risk of HIV acquisition, the association for unstable housing (cRR 1·82 [1·13–2·95; p=0·014]; n=5) was higher than for homelessness (1·44 [1·13–1·83; p=0·0036]; n=12), whereas no difference was seen between these outcomes for risk of HCV acquisition (1·72 [1·48–1·99; p<0·0001] for unstable housing, 1·66 [1·37–2·00; p<0·0001] for homelessness).
Related collections
Most cited references98
- Record: found
- Abstract: not found
- Article: not found
Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement.

- Record: found
- Abstract: found
- Article: not found
Prevention of HIV-1 infection with early antiretroviral therapy.
Author and article information
Comments
Comment on this article
 Smart Citations
Smart CitationsSee how this article has been cited at scite.ai
scite shows how a scientific paper has been cited by providing the context of the citation, a classification describing whether it supports, mentions, or contrasts the cited claim, and a label indicating in which section the citation was made.