- Record: found
- Abstract: found
- Article: found
Trajectories of health care service utilization and differences in patient characteristics among adults with specific chronic pain: analysis of health plan member claims
Abstract
Introduction
The lack of consistency surrounding the diagnosis of chronic non-cancer pain, treatment approaches, and patient management suggests the need for further research to better characterize the chronic non-cancer pain population.
Objective
The purpose of this study was to identify distinct trajectories of health care service utilization of chronic non-cancer pain patients and describe the characteristic differences between trajectory groups.
Patients and methods
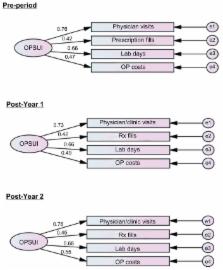
This study utilized the MarketScan claims databases. A total of 71,392 patients diagnosed with either low back pain or osteoarthritis between 2006 and 2009 served as the study sample. Each subject’s claims data were divided into three time periods around an initial diagnosis date: pre-period, post-Year 1, and post-Year 2. Subjects were categorized as either high (H) or low (L) cost at each post period, resulting in the creation of four trajectory groups based on the post-Year 1 and 2 cost pattern: H-H, H-L, L-H, and L-L. Multivariate statistical tests were used to predict and discriminate between trajectory group memberships.
Results
The H-H, L-H, and H-L groups each utilized significantly greater pre-period high-cost venue services, post-Year 1 outpatient services, and post-Year 1 opioids compared to the L-L group ( P < 0.001). Additionally, the H-H and L-H groups displayed elevated Charlson comorbidity index scores compared with the L-L group ( P < 0.001), with each showing increased odds of having both opioid dependence and cardiovascular disease diagnoses ( P < 0.01).
Conclusion
This study identified patient characteristics among chronic pain patients that discriminated between different levels of post-index high-cost venue service utilization and trajectories of change in the same. With implications for managed care program implementation and resource management, this study highlights results from a developed algorithm that employed a variety of accessible data elements to effectively discriminate between patients based on their pattern of high-cost venue service utilization over time.
Most cited references22
- Record: found
- Abstract: found
- Article: not found
Clinical guidelines for the use of chronic opioid therapy in chronic noncancer pain.
- Record: found
- Abstract: found
- Article: not found
Treatment of chronic non-cancer pain.
- Record: found
- Abstract: found
- Article: not found